 |
| Image from Lipoedema Australia Support Society (LASS) |
In lipedema (also spelled lipoedema), the fat cells in certain parts of the body experience overgrowth. It results in an abnormal accumulation of fat, particularly in the lower half of the body; often the arms are affected too.
As we have discussed, lipedema is rarely recognized by doctors, despite being discovered 75 years ago. Often it is thought to be simple obesity, or it is confused with "lymphedema," the accumulation of lymph fluid in the interstitial areas. Because secondary lymphedema can be a late consequence of lipedema, lipedema and lymphedema treatments have often overlapped.
In Part One of this series, we discussed the typical features of lipedema and how differentiate between lipedema and lymphedema.
In Part Two of the series, we discussed how lipedema progresses, the different stages of progression, and why it's so important to be aware of lipedema
In Part Three of the series, we discussed the different types of fat distribution patterns, looked at some pictures to illustrate type and stage of lipedema, and detailed how lipedema is diagnosed.
In Part Four of this series, we examined possible causes of lipedema, as well as medical conditions often associated with it.
Now, in Part Five, we will discuss possible treatments for lipedema in detail. Because we want to give more detail about each option, we are breaking the treatments into several sub-posts:
- Traditional Treatments
- "Weight Control" and Special Nutritional Approaches (trigger warning)
- Tumescent Liposuction
- Alternative Medicine Treatments
Treatment of Lipedema: Overview
The progression of lipedema is highly variable. While the traditional medical teaching is that lipedema is always progressive, some people report that they have been able to stop or even achieve "remission" from lipedema with certain treatments. On the other hand, these reports are anecdotal, and not everyone finds that these treatments help all that much.
You cannot tell how any one case is going to develop over time, and you can't tell what the best treatment will be for any individual. The best thing to do is to keep your options open and explore several different modes of treatment.
As we discuss the options available, remember that the main goals of lipedema treatment are to:
- Minimize discomfort
- Slow/arrest the worsening of the condition
- Prevent secondary lymphedema
- Maintain mobility and everyday functions
There are no pills you can take to fix lipedema, and there are not a lot of highly effective traditional medical treatments at this time. Nothing will cure or reverse it.
However, you may be able to arrest lipedema's progression or minimize the complications. This is VERY IMPORTANT because lipedema can become very disabling.
Most of the traditional treatments were designed to improve lymph flow or reduce swelling. Some have been shown to be quite helpful, while others have been discredited. These treatments have included:
However, you may be able to arrest lipedema's progression or minimize the complications. This is VERY IMPORTANT because lipedema can become very disabling.
Most of the traditional treatments were designed to improve lymph flow or reduce swelling. Some have been shown to be quite helpful, while others have been discredited. These treatments have included:
- Manual Lymph Drainage
- Compression garments, bandages, and pumps
- Complete Decongestive Therapy
- Exercise
- Lymph Node Transplant
- Diuretics
Manual Lymph Drainage Treatments
Because accumulated fat in lipedema can put pressure on lymph vessels and interfere with its free flow, swelling and secondary lymphedema can be side effects of lipedema. Therefore, one of the first recommendations of many doctors is to do Manual Lymph Drainage Treatments (MLD).
There is good evidence that treatment with MLD can reduce edema and leg volume, and perhaps also reduce capillary fragility, resulting in less bruising and fluid accumulation. Small, short-term research has also shown improvement in pain levels for some patients.
Pictures often show dramatic differences in leg size before and after MLD in people with lipo-lymphedema. The woman in the picture experienced a loss of 65 lbs. of fluid after only 2 weeks of MLD! That's how bad lipo-lymphedema can be in some cases.
The most important benefit to Manual Lymph Drainage is that it reduces swelling. This keeps lymph flow as efficient as possible, which in turn may help reduce progression of the disease and improve/sustain mobility. However, while short-term research clearly shows MLD is effective, it usually needs other treatments as well to sustain the benefits long-term.
Anecdotally, there are some impressive success stories of how Manual Lymph Drainage can help, especially those with secondary lymphedema. A trained therapist in your area can be found here or here. But the best results of all seem to come from MLD used with compression. Otherwise, all the benefits of the MLD can be quickly lost.
 |
| Image from mfbewley.org.uk/mld |
 |
| Image from amylhwilliams.com |
The most important benefit to Manual Lymph Drainage is that it reduces swelling. This keeps lymph flow as efficient as possible, which in turn may help reduce progression of the disease and improve/sustain mobility. However, while short-term research clearly shows MLD is effective, it usually needs other treatments as well to sustain the benefits long-term.
Anecdotally, there are some impressive success stories of how Manual Lymph Drainage can help, especially those with secondary lymphedema. A trained therapist in your area can be found here or here. But the best results of all seem to come from MLD used with compression. Otherwise, all the benefits of the MLD can be quickly lost.
Compression Garments, Bandages, and Pumps
One of the hallmark treatments for lipedema is the use of compression bandages, garments, or pumps. They support the tissue and reduce swelling, which reduces pain and leg ache. Compression can be used on its own or used as an adjunct to MLD to help maintain progress.
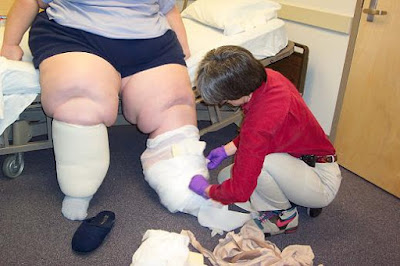
Treatment may be started with bandages at first because compression garments can be too painful for severe cases in the beginning. In the picture above, several layers of bandaging are used and then a compression sock is placed on to of the bandaging.
Another option is intermittent pneumatic compression, which is a pump that inflates and deflates around the leg to compress it. This type of device is often used for patients with chronic lymphedema; its use has been expanded to patients with lipedema too. A doctor's prescription is needed to get a pump, but the good news is that many insurance companies will pay for it.
In the past, pumps were not very efficient and sometimes caused more harm than good to the lymph system. However, newer pumps have been developed that have improved results. Pumps do not replace MLD or compression garments, but they augment other treatments. There are generally two companies who make the pumps, Lympha Press® and Flexitouch®.
There's not a lot of research on the use of pumps for lipedema. One study did not find that the addition of pneumatic compression had any additional benefit over MLD and bandaging. However, anecdotally, many lipedema patients find that they are helped by a pump. You can read more about types of pumps for lipedema here and here.
Knit compression garments are used to keep swelling down on a regular basis. There are many options in compression garments. Those meant for lymphedema may have pressures which are too painful for lipedema patients, who have a greater sensitivity to pain. There is debate over whether flat-knit or round-knit garments are better; according to some, the round-knit can lead to a kind of "tourniquet" effect in some lipedema patients. Others can only tolerate a looser compression garment. The type of garment right for you depends on the stage of lipedema you are in, whether you have large lobes of fat, how large the limb is, and how much pain you have. There are also special sleeves for those with arm lipo-lymphedema.
Some compression garments are not terribly attractive, but others can be more stylish, as seen here. One company that specializes in creating compression garments and products for people with lipedema (as opposed to lymphedema) is lipedemaproducts.com.
You can read more about compression garments here, and the pros and cons of various compression garments here and here. Some people also use garment glue to help keep the compression bandages/garments in place because they can start to get loose and slip as the swelling goes down.
One study suggests "absolutely uncompromising compression therapy" (which sounds rather ominous) for lipedema treatment. However, there are significant barriers to using compression garments.
 |
| Compression bandages and compression sock, Image from amylhwilliams.com |
Treatment may be started with bandages at first because compression garments can be too painful for severe cases in the beginning. In the picture above, several layers of bandaging are used and then a compression sock is placed on to of the bandaging.
 |
| Pneumatic pump for compression |
In the past, pumps were not very efficient and sometimes caused more harm than good to the lymph system. However, newer pumps have been developed that have improved results. Pumps do not replace MLD or compression garments, but they augment other treatments. There are generally two companies who make the pumps, Lympha Press® and Flexitouch®.
There's not a lot of research on the use of pumps for lipedema. One study did not find that the addition of pneumatic compression had any additional benefit over MLD and bandaging. However, anecdotally, many lipedema patients find that they are helped by a pump. You can read more about types of pumps for lipedema here and here.
 |
| Image from lipedemafitness.blogspot.com |
Some compression garments are not terribly attractive, but others can be more stylish, as seen here. One company that specializes in creating compression garments and products for people with lipedema (as opposed to lymphedema) is lipedemaproducts.com.
You can read more about compression garments here, and the pros and cons of various compression garments here and here. Some people also use garment glue to help keep the compression bandages/garments in place because they can start to get loose and slip as the swelling goes down.
One study suggests "absolutely uncompromising compression therapy" (which sounds rather ominous) for lipedema treatment. However, there are significant barriers to using compression garments.
Compression garments are hard to find these in the sizes needed for people with significant lipedema. Often they have to be custom-made to your size. They are expensive, and many insurance companies balk at paying for them (which is ridiculous, considering the cost of treating cellulitis).
Compression garments should be hand-washed daily, and for best results must be worn constantly (you need extra pairs to rotate for washing). They are hot and restrictive, so they are burdensome during the summer. They are difficult and time-consuming to put on, and can restrict activities.
Yet many lipedema patients (especially those with lipo-lymphedema) swear by their usefulness and ability to relieve pain. Many are quite creative in carrying on their daily lives despite the challenges of using compression.
Compression garments are worth trying to see if they help you feel better or lessen swelling. For many, especially those with lymphedema, they are truly a life-saver.
However, no therapy is absolutely required of anyone. You may try it and decide you don't like it, or find it doesn't improve your symptoms. If so, it is certainly your option to discontinue them, or to use them only if symptoms flare. Although compression is a mainstay of most lipedema treatment, it's never compulsory.
Complete Decongestive Therapy
Complex or Complete Decongestive Therapy" (CDT) refers to the package of Manual Lymph Drainage plus compression treatments and sometimes other physical therapy.
It is generally felt that it takes the combination of MLD plus compression to really achieve and sustain real differences in a lipo-lymphedema patient's condition.
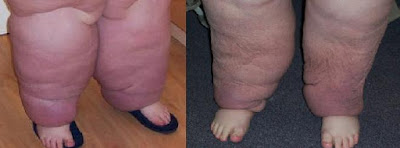
These pictures are of a patient with severe lipo-lymphedema. She lost a total of 60 kg, or about 132 lbs. of fluid, just from CDT treatment over several months. That's how effective CDT can be for people with significant Stage 4 lipedema.
Look how much the lobes on her left leg have been reduced. Notice how much more normal her stance is after the treatment compared to beforehand. I would imagine that helped improve her mobility significantly.
However, not everyone gets these kinds of dramatic results. The more advanced your lipo-lymphedema, the more likely you are to have significant improvement, but all it can do is relieve the worst of the swelling. It cannot reverse lipedema.
In someone with severe lipo-lymphedema, it may be necessary to start treatment slowly because of high pain levels. Very severe cases often start with MLD alone, then add compression bandaging, and then transition into compression garments and pumps as the patient tolerates it. Another alternative may be kinesio taping, which can offer less intense compression.
Bottom line, Complete Decongestive Therapy is the standard of care for treatment of lipedema.
Research and women's stories clearly support CDT as an effective, non-invasive treatment for many people with lipedema.
Compression garments should be hand-washed daily, and for best results must be worn constantly (you need extra pairs to rotate for washing). They are hot and restrictive, so they are burdensome during the summer. They are difficult and time-consuming to put on, and can restrict activities.
 |
| Image from biglegwoman.com |
Compression garments are worth trying to see if they help you feel better or lessen swelling. For many, especially those with lymphedema, they are truly a life-saver.
However, no therapy is absolutely required of anyone. You may try it and decide you don't like it, or find it doesn't improve your symptoms. If so, it is certainly your option to discontinue them, or to use them only if symptoms flare. Although compression is a mainstay of most lipedema treatment, it's never compulsory.
Complete Decongestive Therapy
Complex or Complete Decongestive Therapy" (CDT) refers to the package of Manual Lymph Drainage plus compression treatments and sometimes other physical therapy.
It is generally felt that it takes the combination of MLD plus compression to really achieve and sustain real differences in a lipo-lymphedema patient's condition.
 |
| Before and after 4 months of CDT; Image from Klose and Stroessreuter 2007 |
 |
| Before and after CDT; Klose and Stroessreuter 2007 |
However, not everyone gets these kinds of dramatic results. The more advanced your lipo-lymphedema, the more likely you are to have significant improvement, but all it can do is relieve the worst of the swelling. It cannot reverse lipedema.
In someone with severe lipo-lymphedema, it may be necessary to start treatment slowly because of high pain levels. Very severe cases often start with MLD alone, then add compression bandaging, and then transition into compression garments and pumps as the patient tolerates it. Another alternative may be kinesio taping, which can offer less intense compression.
Bottom line, Complete Decongestive Therapy is the standard of care for treatment of lipedema.
Research and women's stories clearly support CDT as an effective, non-invasive treatment for many people with lipedema.
Exercise
Exercise is crucial to keep lymph flowing well. The lymphatic system doesn't have a pump like the heart (which pumps for the blood vessels).
The lymph system depends on muscle activity and breathing to keep the lymph moving in the body. This means exercise is vital to lipedema patients.
Mobility can be difficult in later stages of lipedema, which means that people exercise less. The lymph system can't pump as well without exercise, and this creates a vicious circle with worsening secondary lymphedema. Regular daily exercise may be particularly important for lipedema patients.
Swimming, water aerobics, and walking in water seem to be the most helpful exercise to folks with lipedema. This is probably because being in water lessens the weight-bearing load, making it easier to move. The pressure of the water can often help force intercellular fluids to even out, so being in water lessens edema. Plus, it just feels good!
Of course, water exercise is not without its challenges. It can be difficult to find a swimsuit in large sizes, it can be expensive to belong to a suitable pool, it can be hard to get in and out of the water in some pools, and some people experience significant public ridicule. Yet water exercise is so freeing that it can be worth the trouble.
Cycling on a stationary bike is another oft-recommended form of exercise for lipedema. Because it can be done seated, less weight is placed on the legs, yet they get plenty of movement to improve blood flow and lymph flow. Of course, it takes money to buy a stationary bike, but many used ones are available cheaply online. Check Craigslist or eBay. Be sure to test it out before you buy it, as there are many variations in design and function and not every model suits every body.
Some people with lipedema really like yoga, especially those in earlier stages. Because yoga involves a lot of deep breathing and strengthening, it can be good for lymph flow and improving muscle tone in people with lipedema. There is even a special type of yoga designed just for improving lymph flow.
However, yoga can be challenging for those with mobility or muscle weakness issues, as well as those with significant swelling or lobes of fat. Sadly, not all yoga teachers are willing to adapt poses for larger bodies or have non-judgmental attitudes towards all bodies.
On the other hand, there are yoga classes that specialize in working with people of size or people with physical challenges. There are also online videos that specialize in yoga for larger bodies.
So while you might encounter some yoga classes that are not welcoming or appropriate for you, don't give up the search. Others might be quite helpful.
Another exercise recommended by some specialists is rebounding. This is a mini-trampoline, preferably with a stability bar.
Rebounding can be especially useful to those who can't do regular exercise because of mobility issues or joint pain. It can also be a good alternative to water exercise, cycling, or yoga for those who have barriers to those activities.
In rebounding, the woman stands on the mini-trampoline, holding on to the stability bar, and gently bounces or "surges" up and down for a few minutes without the feet actually leaving the trampoline.
According to one source, rebounding is particularly helpful because:
High impact exercises like running, jogging, and aerobics are not recommended for lipedema. Sports that involve quick turns and stress on the knees, like tennis, soccer, or skiing, may also be risky. This doesn't mean you can't do them in the early stages, but you need to be very careful. And if your lipedema advances or you start to experience knee issues, you should avoid them. Lipedema strongly predisposes to joint issues and arthritis; an injury could accelerate this process.
Although there are challenges, there are forms of exercise suitable for nearly everyone with lipedema. Even if you are pretty immobile from severe lipo-lymphedema, deep breathing exercises and flexing feet and ankles can help maintain some lymph flow. Another option suggested by some experts is Whole Body Vibration (see below), since this involves just standing on a vibrating platform.
Exercise is not going to make you lose weight, but it may help you maintain your mobility and improve lymph flow in your body. We don't have data to know if it will prevent or delay progression of the lipedema but it seems logical that it might help. Plus, exercise benefits overall health by improving blood sugar, insulin resistance, and cardiovascular health, so it's win-win on several counts.
Keeping as active as your condition permits seems like a common-sense thing to do. Make exercise as much of a priority as you can.
However, it's important to acknowledge that exercise can be quite difficult at a certain stage of progression. Significant creativity may need to be used. But as with every other option, exercise is always a choice, not a requirement.
Lymph Node Transplant
Some women with secondary lymphedema are looking into lymph node transplants, which have helped many women with primary lymphedema. In this, a surgeon takes lymph nodes from another area of your body (usually the neck, armpit, or groin) and transfers them to a trouble area. The blood vessels supporting the lymph nodes are connected to the local blood vessels. In time, these lymph nodes will hopefully start growing new lymph vessels that connect up with other lymph vessels. In this way, doctors hope to improve lymph flow in a badly-affected area.
This is a new technique, mostly used for primary lymphedema or cancer patients. There is not much information on its use in lipo-lymphedema patients, but it's an interesting possibility to keep tabs on for the future.
Diuretics
Diuretics, commonly known as "water pills," are designed to help clear excess fluids from your body. They are typically prescribed for congestive heart failure, lymphedema, or other conditions with chronic edema.
Since many doctors focus mainly on the swelling part of lipedema, they often prescribed diuretics for lipedema patients in the past. Now, however, it is generally recognized that diuretics are very ineffective in treating lipedema.
One review noted that diuretics in lipedema patients may even cause complications:
Exercise is crucial to keep lymph flowing well. The lymphatic system doesn't have a pump like the heart (which pumps for the blood vessels).
The lymph system depends on muscle activity and breathing to keep the lymph moving in the body. This means exercise is vital to lipedema patients.
 |
| Image of Sarah from born2befat.com |
Swimming, water aerobics, and walking in water seem to be the most helpful exercise to folks with lipedema. This is probably because being in water lessens the weight-bearing load, making it easier to move. The pressure of the water can often help force intercellular fluids to even out, so being in water lessens edema. Plus, it just feels good!
Of course, water exercise is not without its challenges. It can be difficult to find a swimsuit in large sizes, it can be expensive to belong to a suitable pool, it can be hard to get in and out of the water in some pools, and some people experience significant public ridicule. Yet water exercise is so freeing that it can be worth the trouble.
Cycling on a stationary bike is another oft-recommended form of exercise for lipedema. Because it can be done seated, less weight is placed on the legs, yet they get plenty of movement to improve blood flow and lymph flow. Of course, it takes money to buy a stationary bike, but many used ones are available cheaply online. Check Craigslist or eBay. Be sure to test it out before you buy it, as there are many variations in design and function and not every model suits every body.
 |
| Photo by Martin Ehleben |
However, yoga can be challenging for those with mobility or muscle weakness issues, as well as those with significant swelling or lobes of fat. Sadly, not all yoga teachers are willing to adapt poses for larger bodies or have non-judgmental attitudes towards all bodies.
On the other hand, there are yoga classes that specialize in working with people of size or people with physical challenges. There are also online videos that specialize in yoga for larger bodies.
So while you might encounter some yoga classes that are not welcoming or appropriate for you, don't give up the search. Others might be quite helpful.
 |
| Image from needakrebounders.com |
Rebounding can be especially useful to those who can't do regular exercise because of mobility issues or joint pain. It can also be a good alternative to water exercise, cycling, or yoga for those who have barriers to those activities.
In rebounding, the woman stands on the mini-trampoline, holding on to the stability bar, and gently bounces or "surges" up and down for a few minutes without the feet actually leaving the trampoline.
According to one source, rebounding is particularly helpful because:
Rebounding (mini-trampoline) causes core muscles and large muscle groups to contract, resulting in the rhythmic compression of the veins and arteries, which more effectively moves fluids, both blood and lymphatic, through the body and back to the heart, lowering peripheral blood pressure and lightening the heart's load...
The up and down motion effectively opens and closes the millions of one-way valves found within our Lymphatic Systems...Most of our valves are positioned vertically, hence vertical motion is favorable simply due to our anatomy. For example, interstitial fluid from the lower extremity is moved upward where it is filtered and finally drained back into the blood in a particular location, up at the clavicle level. ("Thoracic Duct" of the Lymphatic System, our internal vacuum cleaner.)However, some have raised the concern that there really aren't any clinical trials to see if rebounding actually helps or harms.
High impact exercises like running, jogging, and aerobics are not recommended for lipedema. Sports that involve quick turns and stress on the knees, like tennis, soccer, or skiing, may also be risky. This doesn't mean you can't do them in the early stages, but you need to be very careful. And if your lipedema advances or you start to experience knee issues, you should avoid them. Lipedema strongly predisposes to joint issues and arthritis; an injury could accelerate this process.
Although there are challenges, there are forms of exercise suitable for nearly everyone with lipedema. Even if you are pretty immobile from severe lipo-lymphedema, deep breathing exercises and flexing feet and ankles can help maintain some lymph flow. Another option suggested by some experts is Whole Body Vibration (see below), since this involves just standing on a vibrating platform.
Exercise is not going to make you lose weight, but it may help you maintain your mobility and improve lymph flow in your body. We don't have data to know if it will prevent or delay progression of the lipedema but it seems logical that it might help. Plus, exercise benefits overall health by improving blood sugar, insulin resistance, and cardiovascular health, so it's win-win on several counts.
Keeping as active as your condition permits seems like a common-sense thing to do. Make exercise as much of a priority as you can.
However, it's important to acknowledge that exercise can be quite difficult at a certain stage of progression. Significant creativity may need to be used. But as with every other option, exercise is always a choice, not a requirement.
Lymph Node Transplant
Some women with secondary lymphedema are looking into lymph node transplants, which have helped many women with primary lymphedema. In this, a surgeon takes lymph nodes from another area of your body (usually the neck, armpit, or groin) and transfers them to a trouble area. The blood vessels supporting the lymph nodes are connected to the local blood vessels. In time, these lymph nodes will hopefully start growing new lymph vessels that connect up with other lymph vessels. In this way, doctors hope to improve lymph flow in a badly-affected area.
This is a new technique, mostly used for primary lymphedema or cancer patients. There is not much information on its use in lipo-lymphedema patients, but it's an interesting possibility to keep tabs on for the future.
Diuretics
Diuretics, commonly known as "water pills," are designed to help clear excess fluids from your body. They are typically prescribed for congestive heart failure, lymphedema, or other conditions with chronic edema.
Since many doctors focus mainly on the swelling part of lipedema, they often prescribed diuretics for lipedema patients in the past. Now, however, it is generally recognized that diuretics are very ineffective in treating lipedema.
One review noted that diuretics in lipedema patients may even cause complications:
Diuretics can quickly deplete lymphedema fluid but concentrate protein in edematous tissue promoting fibrosclerosis. Use of diuretics in lipedema before lymphedema may result in the development of pseudo Barrter's syndrome characterized by hypokalemic-hypochloremic alkalosis, hyperactivity of the renin-angiotensin-aldosterone system and elevation of atrial natriuretic peptide.Despite the fact that swelling is involved in lipedema, don't let anyone talk you into taking diuretics. Swelling is not the root of the problem; it is only a side effect. Diuretics do not help and may well harm the lipedemic patient.
Most doctors prescribe traditional treatments for lipedema. The most effective seems to be Complete Decongestive Therapy, which includes Manual Lymph Drainage plus some form of compression (bandaging, pumps, or compression garments). There is good research that shows that CDT is modestly effective in lessening the impact of lipedema, so this is probably one of the first treatments that should be considered.
However, should this be the only mode of treatment? Some lipedema websites make the valid point that lymphedema specialists have been the ones discovering and treating most lipedema patients. This means that they may have an unconscious bias towards seeing everything through a lymphedema lens, possibly blinding them to other options. They say:
Historically, lymphedema doctors were early to discover lipedema and unfortunately adopted it as an orphan lymph disorder. These doctors say lipedema is incurable. They say lipedema has progressive stages that once arrived at cannot be reversed. They say treating it with lymphedema protocols is the appropriate approach, not to cure, but to give relief as bodies swell inevitably and painfully to end stage. Without question or research, the medical community follows along with lymphedema doctors' untested assumptions.
As a result, some lipese accept that there is no cure and receive standard lymphedema treatments. These lipese do not improve without daily intervention; expensive wraps and machines to compress "edema" through the lymphatic system. Other lipese say: "Give us clinical trials before you tell us we are incurable."
Consequently, while waiting for real research, many of us have begun to discover and to share ways we treat lipedema successfully, meaning we put ourselves in remission. We have succeeded in improving our lives. We have taken our bodies and minds back. We look forward to our future, not free of lipedema, but rather free of the specter of stages we "must" progress towards.If you look at the traditional treatments discussed in this post, you can see that most of them are indeed aimed at lessening symptoms of lymphedema. But what if we go beyond the lymphedema focus? What other treatments are helpful?
Despite the fact the lipedema has been known about for 75 years, there is limited research on what works best. As a result, people are experimenting with many different treatments. In our next posts, we will explore a few more of these.
For example, many doctors recommend special nutritional diets to lose or "control" weight and reduce symptoms of lipedema. We will examine these suggestions in our next post ─ NOT with the idea of promoting them but with the goal of examining the actual evidence for such recommendations. [Those who find any mention of weight loss or dieting triggering may want to skip that post. It will be the only post covering this, so be sure to return for the next posts in the series.]
One of the most exciting new directions in lipedema treatment is lymph-sparing tumescent liposuction, and our third Treatments post will be on this. While bigger and longer studies are needed, what research we have on this new type of liposuction is very promising so far.
Other women are using treatments from alternative medicine to help their lipedema, and our fourth Treatments post will be on this.
While traditional treatments are primarily aimed at reducing secondary lymphedema, there are other options for lipedema patients. In the next few posts, we will spend time looking at these other options and what research exists on their efficacy.
Again, consult your healthcare provider for their advice, do your own research, and experiment to find what works best for YOU.
References and Resources
Information Resources
*Trigger Warning: Many of these sites are not size-friendly. However, because they also contain valuable information about lipedema and its treatment, they are included here.
- http://www.curelipedema.org/# - Cure Lipedema, lots of info on treatment choices
- http://www.lipomadoc.org/lipedema.html - Website of Karen Herbst, PhD, MD, an endocrinologist practicing in Arizona and one of the most pre-eminent researchers on lipedema
- http://fatdisorders.org/fat-disorders/lipedema-lipoedema-description - Website of the Fat Disorders Research Society
- http://www.nhs.uk/conditions/lipoedema/Pages/Introduction.aspx - United Kingdom's NHS website page on Lipedema
- http://www.hanse-klinik.de/englisch/Lipoedema.pdf - article on lipedema from one of the foremost clinics in Germany that treats lipedema
- http://www.lipv.nl/zslnokycordero.pdf - journal article about lipedema with many pictures
- http://www.lymphedemablog.com/2012/12/13/a-closer-look-at-lipedema-and-the-effects-on-the-lymphatic-system/ - Effect of lipedema on the lymphatic system
- http://www.thelymphoedemacliniclondon.co.uk/pages/treatment-for-lipedema-and-lipo-lymphoedema.php - treatment options for lipedema and lymphedema
- http://blog.wegohealth.com/2014/09/15/the-phases-of-a-lipedema-diagnosis/ - Guide to navigating a lipedema diagnosis, written by Sarah Bramblette, a prominent lipedema activist
- http://www.lipoedemaladies.com/ - International support group for lipedema
- http://www.lass.org.au/ - Lipoedema Australian Support Society (LASS)
- http://www.talklipoedema.org/ - U.K. support and information group for lipedema
- http://www.lipoedema.co.uk/ - U.K. charity to educate about lipedema
- https://www.facebook.com/pages/Lipoedema-Lipedema-Canada-Lipo%C3%A8deme/343801722392863 - Canadian support group for lipedema
- https://www.facebook.com/LipedemaLipoedemaGroupoftheUnitedStates - U.S. Lipedema group
- http://www.lipoedem-hilfe-ev.de/ - German lipedema site (in German)
- http://www.lipoedeemdag.com/ - Dutch lipedema site (in Dutch)
- https://groups.yahoo.com/neo/groups/lipedema_lipodema_lipoedema/info - Yahoo support group, emphasizing research and evidence-based treatments
- https://www.facebook.com/lilithnixroadtorecovery/posts/537379969717549 - Facebook page of a woman with lipo-lymphedema (this link takes you to her biography and lipedema story)
- https://livingwithlipoedema.wordpress.com/ - a British woman's journey with lipedema, particularly focusing on its emotional effect and the treatments she has tried
- http://www.laurajdavis.com/blog/category/lipolymphedema - one woman's history of lipo-lymphedema, failed attempts at weight loss, and treatment difficulties
Acta Pharmacol Sin. 2012 Feb;33(2):155-72. doi: 10.1038/aps.2011.153. Rare adipose disorders (RADs) masquerading as obesity. Herbst KL. PMID: 22301856
...People with RADs [Rare Adipose Disorders] do not lose SAT [subcutaneous adipose tissue] from caloric limitation and increased energy expenditure alone...Treatment recommendations focus on evidence-based data and include lymphatic decongestive therapy, medications and supplements that support loss of RAD SAT....Lymphology. 2008 Mar;41(1):40-4. Complete decongestive physiotherapy with and without pneumatic compression for treatment of lipedema: a pilot study. Szolnoky G1, Borsos B, Bársony K, Balogh M, Kemény L. PMID: 18581957
...We studied whether complete decongestive physiotherapy (CDP) alone or combined with intermittent pneumatic compression (IPC) could improve the treatment outcome in women with lipedema using a prospective, randomized trial. Eleven patients received CDP (60 min) and thirteen CDP (30 min) plus IPC (30 min) once daily in a 5-day-course. Subsequent to drainage, all subjects received multilayered compression bandaging, physical exercise and skin care. Treatment efficacy was evaluated by limb volume reduction. Both groups achieved significant reductions in mean lower extremity volume (p < 0.05). The addition of IPC is safe, although it provides no synergistic benefit to CDP in leg volume reduction under these study conditions.Lymphology. 2011 Dec;44(4):178-82. Lymphedema treatment decreases pain intensity in lipedema. Szolnoky G1, Varga E, Varga M, Tuczai M, Dósa-Rácz E, Kemény L. PMID: 22458119
Lipedema is a disproportional obesity featuring light pressure-induced or spontaneous pain. On the basis of our clinical observations, lymphedema therapy, as practiced in our clinic, reduces the perception of pain beyond leg volume reduction. We therefore aimed to measure pain intensity prior and subsequent to treatment. 38 women with lipedema were enrolled in the study with 19 patients undergoing treatment and 19 serving as the control group using exclusively moisturizers. Treatment consisted of once daily manual lymph drainage (MLD), intermittent pneumatic compression (IPC), and multilayered short-stretch bandaging performed throughout a 5-day-course. Pain was evaluated with a 10-item questionnaire, a pain rating scale (PRS), and the Wong-Baker Faces scale. Treatment resulted in a significant reduction of pain with a decrease in mean scores of all three measures. In the control group, only PRS showed significant decrease. Our study results indicate that this treatment regimen not only reduces leg volume and capillary fragility, but also improves pain intensity in patients with lipedema.Int J Low Extrem Wounds. 2014 Oct 17. pii: 1534734614554284. [Epub ahead of print] Lipedema: A Review of the Literature. Okhovat JP1, Alavi A2. PMID: 25326446
...The current literature suggests that lipedema appears to be a clinical entity thought to be related to both genetic factors and fat distribution. While distinct from lymphedema and obesity, there are some existing treatments such as complex decongestive physiotherapy, liposuction, and laser-assisted lipolysis. Management of lipedema is complex and distinct from lymphedema. The role of newer randomized controlled studies to further explore the management of this clinical entity remains promising.
3 comments:
After a long research my opinion is that Graduated Compression Stockings are play an important role for your fitness.
Excellent article and summation of Lipedema. Thank you :)
Hi, thank you for sharing this great info. Was just browsing through the net in my office and happened upon your blog. It is really very well written and quit comprehensive in explaining with a very simple language.
dystonia pain relief
Post a Comment