September is PCOS Awareness Month. For several years this blog has had an ongoing series about different aspects of PCOS (Polycystic Ovarian Syndrome) and its treatments. Today let's talk about a tough subject: PCOS and hair loss (alopecia).
In our past PCOS series, we have discussed the definition and symptoms of PCOS, how it presents, its testing and diagnosis, and its possible causes. We've also discussed the increased risk for endometrial cancer among those with PCOS.
Now we are discussing common treatment protocols for PCOS, and the pros and cons of each. We've already discussed insulin-sensitizing medications like metformin, the TZDs, and inositol. Then we discussed glucose-lowering medications for those who have developed overt diabetes.
We have also discussed anti-androgenic medications and progesterone supplements for menstrual irregularity. In addition, we did a 3-part series on birth control pills for PCOS.
Now it's time to talk about one of the least-discussed symptoms of PCOS, alopecia (commonly known as hair loss). Today we'll discuss what alopecia is, how it's diagnosed, and what might cause it. In the next post, we'll discuss some of the medical treatments available for it. Finally, we'll discuss some of the cosmetic treatments that women with hair loss may utilize, based on suggestions found on hair loss forums and PCOS boards.
If you have personal experience or expertise in any of these areas, please share in the comments section. Don't let other women walk this path alone; speak up and share your ideas. You are welcome to do so anonymously if you prefer. All comments should be respectful.
The Undiscussed PCOS SymptomNow we are discussing common treatment protocols for PCOS, and the pros and cons of each. We've already discussed insulin-sensitizing medications like metformin, the TZDs, and inositol. Then we discussed glucose-lowering medications for those who have developed overt diabetes.
We have also discussed anti-androgenic medications and progesterone supplements for menstrual irregularity. In addition, we did a 3-part series on birth control pills for PCOS.
Now it's time to talk about one of the least-discussed symptoms of PCOS, alopecia (commonly known as hair loss). Today we'll discuss what alopecia is, how it's diagnosed, and what might cause it. In the next post, we'll discuss some of the medical treatments available for it. Finally, we'll discuss some of the cosmetic treatments that women with hair loss may utilize, based on suggestions found on hair loss forums and PCOS boards.
If you have personal experience or expertise in any of these areas, please share in the comments section. Don't let other women walk this path alone; speak up and share your ideas. You are welcome to do so anonymously if you prefer. All comments should be respectful.
Disclaimer: I am not a medical health-care professional. This information is not medical advice about a health condition or treatment. Consult your healthcare provider before making any decisions about your care.
Irregular periods, sub-fertility, and excess body and facial hair (hirsutism) are the classic symptoms of PCOS, and the ones that get discussed the most on PCOS publications and boards. Acne, weight gain, insulin resistance, and blood sugar issues are other symptoms that get discussed regularly.
However, one of the least-discussed symptoms of PCOS is hair loss (androgenetic alopecia). Even acanthosis nigricans and skin tags get more discussion time on PCOS boards than hair loss.
Sadly, alopecia (and how to deal with it) is not discussed very openly, even among women with PCOS. Sometimes it's simply because the majority of women with PCOS do not experience hair loss, but often it's because of the very strong stigma of hair loss in women. Women simply do not want to admit publicly that they are experiencing hair loss, or they may be in denial about it.
For those who do experience hair loss, it's heartbreaking. Facial hair can be shaved off, but significant hair loss on the scalp is extremely difficult to deal with in a society that judges a woman on her appearance (especially her hair, her so-called "crowning glory"). Shame and embarrassment are common feelings among women with hair loss. "Fixing it" becomes the focus.
Some types of hair loss are fixable, but not all. It's important to acknowledge that up front. Unfortunately, right now there is not a lot that can be done for the type of thinning hair that comes with PCOS except to slow it down. PCOS hair loss is typically caused by the skin being ultra sensitive to androgens. Androgen-blockers can sometimes help, but in most cases, treatment for women with PCOS hair loss only results in slowing down or covering up the hair loss, not reversing it.
However, this does not mean that women with PCOS are without choices. There are many different ways of approaching alopecia, and many ways you can still have a great life despite the PCOS and alopecia. Don't let it stop you or silence your voice.
Types of Alopecia
First, it's important to understand what alopecia is, so let's start with a primer on women's hair loss.
There are many types of alopecia. Some are treatable and some are not, so it's important to know which type you have. Here are a few of the possibilities.
Alopecia Areata
Alopecia Areata (AA) is a patchy type of hair loss, rather than the overall thinning on top of the head seen with the Androgenetic Alopecia of PCOS. It often comes on quickly and results in small circular bald patches. Both men and women can experience it. According to some sources, a person has about a 2% chance of developing AA at some point during their lifetime.
 |
| Actor Matt Lucas, wikimedia commons |
Alopecia Areata is due to an autoimmune condition, and as a result can come and go in severity:
In alopecia areata, immune system cells called white blood cells attack the rapidly growing cells in the hair follicles that make the hair. The affected hair follicles become small and drastically slow down hair production. Fortunately, the stem cells that continually supply the follicle with new cells do not seem to be targeted. So the follicle always has the potential to regrow hair.
Scientists do not know exactly why the hair follicles undergo these changes, but they suspect that a combination of genes may predispose some people to the disease. In those who are genetically predisposed, some type of trigger–perhaps a virus or something in the person’s environment–brings on the attack against the hair follicles.The good news for people with AA is that the condition is usually temporary. They have the hope of their hair growing back at some point. For most, the hair returns, but for some, the hair never does come back. Or their hair may come and go unpredictably through their lives, and they never quite know what to expect.
Mild AA can be fairly easy to deal with, from simply styling the hair a different way or applying a little scalp concealer. However, it can be very difficult to deal with severe AA, especially Alopecia Totalis or Universalis. Dealing with the loss of eyebrows and eyelashes as well as complete baldness on top is not easy, especially for women.
On the other hand, some deal with the loss quite effectively with wigs, false eyelashes, eye liner, or tatooed-on eyebrows. There are many resources for products like these here. Some celebrities have had AA and successfully hidden it, like Christopher Reeve and Neve Campbell.
Others choose not to hide their condition, like actor Matt Lucas or athlete Charlie Villanueva. They find trying to hide it a waste of time and energy and live proudly bald.
Here are some links for further information about AA:
- http://www.niams.nih.gov/Health_Info/Alopecia_Areata/default.asp
- http://www.americanhairloss.org/types_of_hair_loss/alopecia_areata.asp
- http://www.baldgirlsdolunch.org/ - also check out their Facebook page
- www.alopeciaareataresearch.com
- http://www.7billionones.org/nicole
- https://healthresearchfunding.org/famous-people-alopecia/
- www.naaf.org - National Alopecia Areata's main website
- https://www.facebook.com/NAAFUSA/posts/208447452569485 - National Alopecia Areata Foundation's Facebook page
- If Your Hair Falls Out, Keep Dancing! How to Cope with Alopecia Areata in a Hair-Obsessed World - by Leslie Ann Butler. Available here
- Boldly Bald Women by Pam Fitros. Available here
- Blonde today, Bald Tomorrow: Living Life with Alopecia - by Stacy Weed. Available here
Telogen Effluvium (TE) is a temporary form of hair loss and will usually resolve. It usually occurs as the result of a shock, crisis, or drastic hormonal change in the body.
Normally, hair does not continually grow on the scalp. It goes through a growing phase ("anagen") and a resting phase ("telogen"). Normally, about 10-20% of the hair follicles on your head are in a resting phase at any one time. Telogen Effluvium occurs when something causes a higher percentage of follicles to go into telogen phase, making the hair look thinner. Usually this resolves within a few months, but sometimes it takes longer or becomes chronic.
One common cause of TE is from medication which changes hormone levels, such as starting or stopping hormonal birth control like oral contraceptives. TE can also result from hormone replacement therapy, Clomid, or steroid use. Some medications for blood pressure, diabetes, hypothyroidism, anti-depressants, or high cholesterol can also cause temporary hair loss.
Probably the most common cause of TE is post-pregnancy hormone changes. The high estrogen levels of pregnancy can cause thicker and more plentiful hair, but once the estrogen levels drop after childbirth, the extra thickness and hair is lost as most of the hair goes into a "resting" phase, making the hair appear thin. It may take a while for hair to normalize, but most women with post-partum thinning go back to their normal appearance with time.
Some chronic illnesses like Crohn's Disease, IBD (Inflammatory Bowel Disease), hypothyroidism, or liver disease can cause Telogen Effluvium too. A severe shock to the system from things like car accidents, crash diets, severe stress, or serious illnesses can cause it. TE is also common after major surgery in women but may take a while to appear.
Dietary deficiencies are classic causes of TE as well. Common ones include deficiencies in iron, ferritin, biotin, protein, zinc, and certain B vitamins (especially B12), as well as too much vitamin A. Sometimes vegans are prone to hair thinning because over time they may develop a B12 deficiency. Many people who have had gastric bypass or other malabsorptive bariatric surgeries have hair fall out eventually as nutritional deficiencies accumulate over time. Eating disorders can also bring on TE.
Anagen Effluvium
Anagen Effluvium (AE) is a rapid and sudden hair loss from exposure to toxins or treatments for cancer. Chemotherapy is a common source of temporary hair loss for those with cancer because it usually targets all rapidly dividing cells. This means it targets cancer, but hair and mouth cells are also rapidly dividing cells and so are often collateral damage. Radiation treatments to the brain also often cause hair loss.
Although hair usually grows back after chemotherapy and/or radiation, it may grow back differently (changed color, straight instead of curly, change in texture). In some cases, it grows back only partially and never gets back to the fullness it used to have. Sometimes this patchiness can be quite pronounced.
Other Types of Alopecia
There are other, more rare types of alopecia as well, including Scarring Alopecia and Traction Alopecia. These result from trauma to the scalp, usually from tight hairstyles like braids, cornrows, tight ponytails, or hair extensions.
Bald spots can also result from trichotillomania, a compulsive pulling of a person's own hair. Infections can cause similiar hair loss, including fungal infections (like ringworm) and folliculitis. Diseases like lupus, congenital adrenal hyperplasia, or syphilis can also result in hair loss. And of course, age causes a gradual thinning of the hair in many people as hormones shift. About half of women experience some degree of hair loss after menopause.
Androgenetic Alopecia
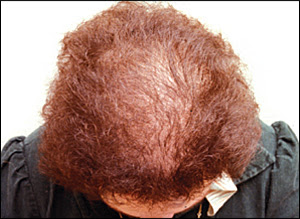 |
| FPHL involves more diffuse thinning |
 |
| Typical male vs. female hair pattern loss differences |
Dihydrotestosterone (DHT), a derivative of the male hormone testosterone, is the main culprit behind hair loss in both men and women, as one website explains:
Testosterone converts to DHT with the aid of the enzyme Type II 5-alpha reductase, which is held in a hair follicle's oil glands. Scientists now believe that it's not the amount of circulating testosterone that's the problem but the level of DHT binding to receptors in scalp follicles. DHT shrinks hair follicles, making it impossible for healthy hair to survive.
The hormonal process of testosterone converting to DHT, which then harms hair follicles, happens in both men and women. Under normal conditions, women have a minute fraction of the level of testosterone that men have, but even a lower level can cause DHT- triggered hair loss in women. And certainly when those levels rise, DHT is even more of a problem. Those levels can rise and still be within what doctors consider "normal" on a blood test, even though they are high enough to cause a problem. The levels may not rise at all and still be a problem if you have the kind of body chemistry that is overly sensitive to even its regular levels of chemicals, including hormones.
Since hormones operate in the healthiest manner when they are in a delicate balance, the androgens, as male hormones are called, do not need to be raised to trigger a problem. Their counterpart female hormones, when lowered, give an edge to these androgens, such as DHT. Such an imbalance can also cause problems, including hair loss.Many women with PCOS experience Androgenic Alopecia, although it is a far less common symptom than hirsutism or acne. Put another way, though hair loss rates are higher in women with PCOS than in the general population, most women with PCOS do not experience hair loss.
Why some women with PCOS experience alopecia and others do not is not clear. It probably has to do with each person's unique genetic make-up, hormone levels, and sensitivity to androgen receptors.
Summary
The bottom line is that there can be many causes of hair loss. Just because you have PCOS does not mean you could not possibly develop Alopecia Areata or have hair loss due to an underactive thyroid or a nutrient deficiency. You need to have your case reviewed by a dermatologist so you can get to the bottom of the cause of your hair loss.
Many types of hair loss are treatable and reversible, but some are not. Unfortunately, Androgenetic Alopecia, the type most common with PCOS, does not usually seem to be reversible, but there may be things you can do to slow it down. And of course, there are many practical things you can do to disguise it, if you wish to do so. Or you can simply learn to deal with the hair loss and not let it affect your happiness.
How Common is Hair Loss in PCOS?
One difficult question to answer is the incidence of alopecia in women with PCOS.
There is plenty of research documenting how much of the overall population experiences hair loss at some point in their lives, but most of this research does not differentiate between causes of the hair loss, just that it occurs at some point.
It is very difficult to separate out figures of alopecia in the general female population vs. those that are attributable to PCOS alone. First, let's start by discussing alopecia in the female population by age.
Hair Loss by Age
Most research focuses on the prevalence of hair loss differentiated by age. For example, it is estimated that about one-fourth of men begin balding by age 30, but that this increases to about two-thirds by age 60.
In women, the numbers are more uncertain. One study found that about one-third of all Caucasian women experience female-pattern hair loss (FPHL) at some point; however, a lot of this hair loss occurs after menopause. How much occurs before menopause is less clear.
One study found that about 10% of pre-menopausal women experience significant hair loss, and this number increases to about 50-75% of women over age 65. Another study found hair loss rates of about 12% of women in their 20s, which increased to 57% in women over age 80:
Twelve percent of women first develop clinically detectable FPHL by age 29 years, 25% by age 49 years, 41% by 69 years, and over 50% have some element of FPHL by 79 years. Only 43% of women aged 80 years and above show no evidence of FPHL.How many of these women might have PCOS? It's not clear. One study of Finnish women found that about one-third experienced noticeable hair loss by age 63, and that this hair loss was often tied to strong insulin resistance. The more severe the degree of hair loss, the more severe the insulin resistance the woman likely had. Thus, it's likely that many of these women had PCOS, but the study did not look into that connection directly.
Alopecia Incidence in Women with PCOS
We do know that alopecia and PCOS are tightly tied together. One study showed that two-thirds of women experiencing hair loss had PCOS.
But this doesn't tell us the opposite; how many women with PCOS experience hair loss as one of their symptoms?
Not a lot of research exists on this question. Most studies do not quantify how many women with PCOS also have alopecia, just that it's a relatively uncommon symptom. However, recently some data has emerged, although the sample sizes in the studies are fairly small so the results vary considerably.
One British study (Sivayoganathan, 2011) found that 16% of women presenting with PCOS-like symptoms had hair loss, whereas 56% had hirsutism.
Another slightly larger study (Quinn 2014) found that 22% of women who met strict criteria for PCOS were experiencing alopecia.
Another study (Ozdemir 2010) found that 34.8% of women with PCOS had alopecia, whereas 73.9% of them had hirsutism. Similarly, Christodoulopoulou 2016 found that 36% of women with PCOS experienced alopecia.
So while most women with PCOS do not experience alopecia, between 16-36% do. In other words, between 1 in 6 and 1 in 3 women with PCOS experience hair loss. Yet even among this group, hair loss is largely ignored or talked about only minimally because of the shame and embarassment.
Interestingly, while hirsutism seems to be fairly closely correlated with androgen levels, alopecia does not. It may be less about how much androgens you produce and more about how sensitive your hair follicles are to androgens. This raises the question of whether anti-androgen medications are really an effective treatment for alopecia. (More on that in another post.)
Diagnosing Alopecia
 |
| The Ludwig Scale of Female Pattern Hair Loss (1977) |
The progression of female-pattern hair loss is usually judged on either the 3-point Ludwig Scale (above), the gradated 3-point Savin Scale (see the bottom of this section), or the 5-point Sinclair Scale (see just below). While there are other scales available, the Ludwig or Sinclair scale seems to be the most commonly used.
 |
| Sinclair Scale for hair loss |
Research strongly suggests that tests for nutritional and endocrine issues also be run, including:
- DHEAs
- Testosterone
- Androstenedione
- Prolactin
- Follicular stimulating hormone
- Leutinizing hormone
- Serum iron
- Serum ferritin
- Total iron binding capacity (TIBC)
- Thyroid stimulating hormone (T3, T4, TSH)
- VDRL (a screening test for syphilis)
- Complete blood count
- Zinc, Vitamin D
 |
| Savin Scale of hair loss |
Rarely do women with androgenetic alopecia lose all their hair, have a completely receding front hair line, or have complete bald spots. Instead, the hair becomes progressively thinner and more diffuse, and the scalp shows through more and more, especially in direct light. Eventually, this hair loss can become severe and become near-baldness, especially as women pass menopause.
Women's AGA alopecia tends to become noticeable later than in men, but because they are more conscious of their hair and because the social ramifications of hair loss are more severe, they tend to come in for diagnosis and treatment earlier in the process.
While hair loss is emotionally difficult for both genders, it is especially traumatic for women. Hair loss in men is common and baldness is relatively accepted; in women, it is highly stigmatized, so it is nearly always hidden away and is rarely discussed.
Summary
There are many forms of alopecia and many possible causes for it.
This is why it's important to see a dermatologist in the early stages of alopecia, so you can hopefully find some answers sooner than later. Unfortunately, many doctors are dismissive of these concerns or just put you on strong medications right away instead of trying to determine the root cause of the issue. Women on the PCOS forums stress the importance of seeing more than one doctor if necessary to get answers.
Once a cause is determined, then a course of treatment can be prescribed. Sometimes this is helpful, often it is not, but it may be worth trying just to see. More on these treatment options in the next posts.
Information is power. Make your decisions from an informed place and be aware that there is a lot of quackery and fraud in the hair loss field. People make all kinds of recommendations and claims about treatments, but very little data exists proving whether these treatments actually help.
Be very wary about claims of what can help, even from PCOS resources. Research as much as you can to learn about the benefits and risks of everything you consider trying. Be sure to visit the hair loss forums online so you can gain wisdom and support from those who have already traveled this path before you.
Above all, remember that your looks don't define you. Women with PCOS have many challenges to their self-esteem via hirsutism, acne, weight, and/or alopecia. Dealing with these challenges is frustrating and demoralizing at times, but ultimately these challenges do not define you. Only you can do that.
Remember that who you are inside is the most important thing, and that your confidence and a strong sense of self can overcome society's prejudices.
Next post: Medications and Treatments for Alopecia
References
J Family Reprod Health. 2016 Dec;10(4):184-190.Clinical and Biochemical Characteristics in PCOS Women With Menstrual Abnormalities. Christodoulopoulou V, Trakakis E, Pergialiotis V, Peppa M, Chrelias C, Kassanos D, Papantoniou N. PMID: 28546817
...MATERIALS AND METHODS: We conducted a prospective observational study of patients 17-35 years of age with PCOS that attended the department of Gynecological Endocrinology of our hospital. RESULTS: A total of 309 women with PCOS participated in the study. In total, 72.2% suffered from menstrual cycle disorders...36% of the sample had androgenetic alopecia and 56.4% had acne....Fertil Steril. 2014 Apr;101(4):1129-34. doi: 10.1016/j.fertnstert.2014.01.003. Epub 2014 Feb 15. Prevalence of androgenic alopecia in patients with polycystic ovary syndrome and characterization of associated clinical and biochemical features. Quinn M, Shinkai K, Pasch L, Kuzmich L, Cedars M, Huddleston H. PMID: 24534277
OBJECTIVE: To describe the prevalence of androgenic alopecia (AGA) in patients with polycystic ovary syndrome (PCOS) and to characterize associated clinical and biochemical features... SETTING: Multidisciplinary PCOS clinic at a tertiary academic center. PATIENT(S): A total of 254 women with PCOS according to the Rotterdam criteria were systematically examined from 2007 to 2012 by a reproductive endocrinologist, a dermatologist, and a psychologist... RESULT(S): Fifty-six of 254 patients with PCOS (22.0%) had AGA. Subjects with PCOS and AGA were more likely to have acne or hirsutism than those without AGA (96.3% vs. 70.6%)... There were no differences between subjects with and without AGA in biochemical hyperandrogenism or metabolic parameters. CONCLUSION(S): AGA is prevalent in 22% of subjects meeting diagnostic criteria for PCOS. AGA is associated with other manifestations of clinical hyperandrogenism, but not with greater risk of biochemical hyperandrogenemia or metabolic dysfunction than with PCOS alone.Hum Fertil (Camb). 2011 Dec;14(4):261-5. doi: 10.3109/14647273.2011.632058. Full investigation of patients with polycystic ovary syndrome (PCOS) presenting to four different clinical specialties reveals significant differences and undiagnosed morbidity. Sivayoganathan D, Maruthini D, Glanville JM, Balen AH. PMID: 22088131
OBJECTIVE: This study aimed to compare the spectrum of polycystic ovary syndrome (PCOS) symptoms in patients from four different specialist clinics. DESIGN: A prospective cross-sectional observational study. SETTING: The study was conducted at the infertility, gynaecology, endocrine and dermatology clinics at Leeds General Infirmary, U.K. PATIENTS: Seventy women presenting with features of PCOS: 20 from infertility, 17 from gynaecology, 17 from dermatology and 16 from endocrine clinics. INTERVENTIONS: Participants were assessed for symptoms and signs of PCOS and underwent a full endocrine and metabolic profile and a pelvic ultrasound scan. RESULTS: All subjects had experienced menstrual problems, 81% were overweight, 86% had polycystic ovaries on ultrasound, 56% had hirsutism, 53% had acne, 23% had acanthosis nigricans, 16% had alopecia and 38% had previously undiagnosed impaired glucose tolerance (IGT) or diabetes....Acta Obstet Gynecol Scand. 2010;89(2):199-204. doi: 10.3109/00016340903353284. Specific dermatologic features of the polycystic ovary syndrome and its association with biochemical markers of the metabolic syndrome and hyperandrogenism. Ozdemir S, Ozdemir M, Görkemli H, Kiyici A, Bodur S. PMID: 19900078
...DESIGN: Prospective descriptive analysis. SETTING: University-based tertiary care. SAMPLE: One-hundred and fifteen untreated consecutive women diagnosed as having PCOS... RESULTS: The prevalence of acne, hirsutism, seborrhea, androgenetic alopecia and acanthosis nigricans was 53%, 73.9%, 34.8%, 34.8% and 5.2%, respectively. Acne was not associated with the hormonal, metabolic and anthropometric variables. Hirsutism had positive associations with total testosterone, fasting glucose and total cholesterol, and a negative association with age. Seborrhea was found to be related with free testosterone, fasting glucose and insulin. A negative association was determined among androgenic alopecia and free testosterone, low-density lipoprotein and insulin. CONCLUSIONS: Acne and androgenic alopecia are not good markers for the hyperandrogenism in PCOS. Hirsutism appears to be strongly related with hyperandrogenism and metabolic abnormalities in PCOS women.


No comments:
Post a Comment