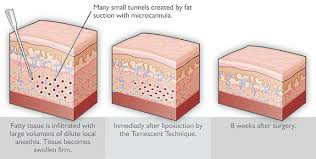
One of the more controversial treatments for lipedema involves liposuction. Some people have had disastrous experiences with it in the past, some swear by the new techniques available for it, and some want to see larger and more long-term research before they come to any conclusions.
In the past, traditional "dry" liposuction with general anesthesia was tried on lipedema patients and often made things worse rather than better. Some developed more secondary lymphedema after these procedures than they had before them.
However, new techniques have been developed that seem to be far more effective and less damaging than the older techniques, and preliminary research is quite promising.
Let's look at liposuction for lipedema in more detail.
Many women who have struggled with the extra bulk of lipedema have secretly wished they could cut away or suck out the extra fat from their bodies. Sadly, many doctors have had this same impulse and tried to do it for years, harming many women in the process.
Lipectomy (cutting away fat pads or lobes) has been tried on lipedema patients with very poor results.
One classic 2012
textbook on lymphology wrote:
Surgical removal of adipose tissue, lipectomy, can cause lymphedema as a complication, because lymph vessels are always removed along with the fat. It is particularly dangerous if fat pads medial to the knee joints are excised - as previously explained, the ventromedial lymph vascular bundle is located in this region. Lymphedema is a much more serious disease than lipedema. People do not die of lipedema, but lymphedema can lead to angiosarcoma.
Liposuction (vacuuming out fat cells) is used for reducing fat to "improve" cosmetic appearance, so many doctors hypothesized that this fat removal would help in lipedema. However, traditional "dry" liposuction is one of the worst things you can do for lipedema. Most don't seem to benefit that much and some even seem to get worse because traditional liposuction techniques can damage the lymph system. As the
translation of one German expert's paper explains:
The results of liposuction using dry suction ranged from disappointing to disastrous. The criss-cross technique used in the dry technique of liposuction, which was reasonable in aesthetic surgery, ended up destroying numerous lymph channels in the lipedema patient, which inevitably lead to a post-surgical lymphedema. Anatomical studies came to the conclusion that lymph vessels are rather robust against sheering powers in a longitudinal direction, but can be easily damaged in a transversal axis. This led to the insight to use suction in the direction of the lymph axis.
Lipectomy and traditional dry liposuction have pretty much been discredited as viable treatments for lipedema. But now there are new techniques in liposuction that have people taking a second look at that option.
Lymph-Sparing Tumescent Liposuction
|
|
Tumescent liposuction. The fluid on the table is from
the injection of fluids under the patient's skin
|
Recently doctors have come up with a new procedure called "Lymph-Sparing Tumescent Liposuction." This is not done in the old "dry" way, but with a new "wet" technique that is thought to be less harmful.
The Procedure
Before the liposuction begins, surgeons usually use standard pre-op procedures like antibiotics, skin cleansing using Hibiclens, and mild anti-anxiety medications. All medications or herbs with anti-coagulant effects should have been stopped well before the surgery (NSAIDs, turmeric, aspirin, etc.).
Once the "wet"
tumescent liposuction begins, fluids containing local
anesthesia (usually lidocaine for pain relief) and
epinephrine (to shrink blood vessels and minimize bleeding) are injected under the skin. The tissue becomes very swollen and firm ("tumescent"), making it easier to separate the fat tissue from the other tissue so it can be removed more easily. Then the surgeons wait a while for the medications to take full effect before proceeding to the next phase.
At this point, a series of small incisions are made. Small vibrating microcannula (mini-tubes) are inserted under the skin in a longitudinal direction to remove fat cells, taking care to avoid blood and lymph systems as much as possible. The vibrating microcannula help separate the fat cells from the other structures in the skin, then use a vacuum in the tube to suction fat cells out. The small incision holes are left open after the surgery so the excess fluid can leak out and disperse. Absorbent bandaging is applied to help soak up the leaking fluids.
Dr. David Greuner, a surgeon in New York City who does this new type of liposuction,
describes it this way:
We are using...a very specialized form of [liposuction] in order to preserve all healthy tissue while removing diseased tissue. The way I like to describe it is very refined meticulous liposuction...There are a lot of tissues that...are particularly important in patients with lipedema or lymphedema. They are the bridging blood vessels, veins, arteries as well as lymphatic channels that drain the skin and fatty tissue on the way to going back into your circulation...if you disrupt this network of very fine, almost invisible blood vessels and lymph vessels you can actually cause a tremendous amount of pain, swelling and delayed feeling for these patients.
Although most capillaries are not damaged in the procedure, there can be some blood in the fluids leaking after the procedure. Bruising may also appear as a result of minor bleeding under the skin. Some doctors also use low molecular weight heparin injections after the procedure to lower the risk for blood clots; these might increase bruising somewhat.
One major advantage of tumescent liposuction is that it does not involve general anesthesia, only topical local anesthetic injected under the skin with fluids. This means less anesthesia for the liver to metabolize, as well as a quicker recovery. In addition, some experts feel that general anesthesia procedures should be avoided when possible in lipedemic patients because they paralyze and shut down the lymphatic system for a while, perhaps predisposing to secondary lymphedema. General anesthesia also involves a higher risk for death and serious complications, especially in "obese" people. The advent of tumescent liposuction with only local anesthesia represents a big step forward in lowering the risk of this procedure, especially in larger people.
Types and Techniques
There are different
technique variations in lymph-sparing liposuction. The most popular currently is
WAL,
Water-jet Assisted Liposuction. Some surgeons seem to consider this a subset of tumescent liposuction techniques, while others seem to consider it a different procedure altogether.
WAL uses
slightly pressurized water jets on the micro-cannula to help
gently separate and remove the fat tissue from the surrounding tissue, which is then suctioned out with the micro-cannula. Research
confirms that this technique is lymph-sparing.
Many liposuction surgeons currently use WAL for their lipedema patients because they feel it is the easiest on the lymph system. They consider WAL the most state-of-the-art liposuction technique for lipedema patients available today.
There is also a version of liposuction that uses lasers to help destroy the fat cells before they are removed. The fat cells are ruptured using the heat from mini-lasers and then suctioned out. Any tissue left behind helps form scar tissue, which is supposed to tighten up lax skin. Some surgeons favor this for arm liposuction in particular.
Ultrasonic liposuction has also been
touted as a treatment for lipedema. It uses ultrasound to help break down the fat before it is suctioned away:
Ultrasonic liposuction works by transmitting shock waves through a special handpiece to the end of a cannula (fine tube), which is inserted into the area to be treated. The waves break up the fat, turning it into a milky emulsion, which is then sucked up by the cannula.
So there are a number of different technique options for lipedema liposuction. It's important to do your research on the pros and cons of each.
At this time, it appears that most lipedema experts prefer using WAL liposuction. They see it as the most effective and least damaging technique available. A few
surgeons will use WAL plus lasers in certain areas. Although the studies on WAL are small, the results are generally quite positive.
Post-Op Care
Post-operative care after tumescent liposuction usually involves bandaging or compression garments 24 hours a day for about a week or so, sometimes lasting a few weeks. Mobility is limited at first, so it's important to have a helper who can do the post-op wound care, bandaging, and compression garments for the first few weeks.
The extra fluids pumped under the skin will slowly leak out for several days post-op, so recovery can be messy. As mentioned, these fluids may be blood-tinged at times, and bruising may also appear. Some patients experience significant itching and tenderness in the area which has been treated, while others aren't affected as strongly.
As soon as you are ready, walking is useful to help the lymph system clear the body of leftover fluids and debris. Walking will be slow and gentle at first but should increase as you recover. With more advanced cases of lipedema, Manual Lymph Drainage may also be used during the recovery period.
Short showers are permitted within a day or so after the procedure, but full bathing, swimming, or other immersion is typically not allowed for several weeks. An oral antibiotic is usually continued for a few days after surgery, and some doctors will also give low molecular weight heparin for a few days or weeks, especially for those traveling long distances after the surgery.
For more details on the pre- and post-op procedures and after-care of one surgeon, see
this article. (Keep in mind that every surgeon will likely have a slightly different protocol.) For one woman's post-op recovery story, read
this and
this. Another woman's journey is chronicled
here. Additional liposuction stories are linked to at the bottom of this post.
Although some people only need one procedure, most people undergo
multiple procedures in order to address all the different areas affected by lipedema without endangering the circulatory system (too much removed at once could cause the circulatory system to collapse). Those with Stage 1 and 2 lipedema can have their procedures performed fairly close together, while those with Stage 3 and 4 lipedema need to space their procedures apart further to allow for sufficient recovery and to get the best results.
Although progress is seen within 2-4 weeks after each procedure, the final results are often not seen for six months to a year, after the body remodels itself. For those with extensive lipedema, additional skin "lift" procedures may be needed to deal with sagging skin afterwards.
Pros and Cons
Like any other treatment, tumescent liposuction for lipedema has pros and cons. Let's look at these more closely.
Pros
Liposuction is the only lipedema treatment to actually remove some dysfunctional fat cells from the body rather than trying to just minimize swelling or improve lymph flow. These fat cells never come back so the mischief they cause (leakage of fluids, impairment of lymph flow, pain, bruising) is gone from the body.
However, liposuction is NOT a cure; it is impossible to remove all lipedemic fat, and whatever causes lipedema is still there and may still cause overgrowth of current fat cells and creation of new ones. In a best-case scenario, however, this procedure can reduce lipedema fat considerably and lessen pain, bruising, and probably slow progression of the condition.
Remember, lymph-sparing tumescent liposuction doesn't take the lipedema away. At best, it offers a bit of remission, an ability to go back a number of years in the progression of lipedema, regaining some mobility and reducing limb size. This alone can be a tremendous blessing to people with lipedema, enough to justify its risks to many people.
It is also hoped that liposuction will lessen the pressure on the vascular and lymph systems and so prevent or delay the development of lipo-lymphedema. Although this is speculative, it does seem logical and would be a
huge advantage to doing liposuction. Only longer-term research will tell for sure.
Cons
On the other hand, any surgery carries risks of bleeding, infection, and trauma to the area. And if the liposuction is not done well, the lymph system might actually be damaged
more. These risks must be weighed against the possible benefits.
Don't forget to factor in the risks of any additional surgeries that might be required later on. As mentioned, some might need skin "lift" surgeries afterwards, and of course those surgeries also
have risks, especially since they are more invasive and involved than liposuction itself. Abdominal lifts ("panniculectomies") particularly tend to have complicated recoveries.
Another major con is the expense of the surgeries, the fact that insurance rarely covers them, and the reality that most people must travel in order to get lipedema-specific liposuction. That means taking time off work, a helper taking time off work to go with you, and the expense of traveling and living for a while in another city.
Furthermore, the cosmetic results of liposuction for lipedema are not always that impressive. The amount of weight lost from the procedure is minimal, and the cellulite will not disappear. Some patients achieve significant limb volume reduction, but not everyone does. This means that some women who hope for major cosmetic improvements are disappointed in the results. Of course, the main reason to do the procedure is to lessen pain and the pressure on the lymph and vascular systems, not to achieve weight loss or improve cosmetic appearance. It's important to keep expectations realistic and focused on the
real purpose of the surgery.
Are The Results Long-Term?
One of the most critical questions about tumescent liposuction for lipedema is whether the
results are long-term or whether additional fat comes back.
No one really knows the answer to this. We do know that the
fat cells removed in liposuction are gone for good and those fat cells don't come back. However, will others grow in their place later on?
Because lipedema probably involves both
hypertrophy (over-growth of existing fat cells) and
hyperplasia (over-production of new fat cells), our best guess is that it likely will cause significant overgrowth again at some point. Tumescent liposuction merely buys more time, improves quality of life, and hopefully lessens complications.
Until doctors can pinpoint the real underlying cause of fat cell overgrowth (my bet is an endocrine abnormality acting on a genetic predisposition), tumescent liposuction is only a stopgap ─ but it's the only stopgap that offers real hope for significant improvement.
Because tumescent liposuction for lipedema hasn't been done that long, no one knows what the truly long-term results will be. The short- and mid-term results are promising, however.
Results
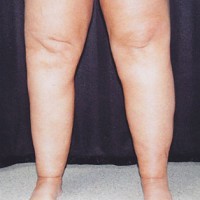
Some people have had some dramatic results with lymph-sparing tumescent liposuction, while others have had only so-so results. Keep in mind that most of the pictures available online are of the most-impressive results; your results might not be so dramatic. Here are some of the more impressive ones.
Before and After Pictures
|
|
Before and After images from Schmeller 2012
|
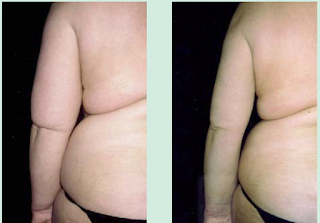
Schmeller et al., 2012, reported on their results with WAL liposuction in Germany over several years, and included pictures of some of the more dramatic cases. In the picture above, a 42 year-old woman had 4 different WAL liposuction procedures done (hips, buttocks, thighs, and lower leg), and the differences are quite marked nearly 2 years after the first surgery.
|
|
Image also from Schmeller 2012
|
In another case from the same study, a 34 year-old woman had 1 liposuction procedure done, focusing on the lower legs. Again, even 3 years after the procedure, the difference is quite marked.
Another impressive before-after case is Jasna Turnic, a patient who had the surgery done in L.A., and who documented it in a report
here. She was probably only Stage 2, but she was already experiencing significant pain and mobility issues. Her legs look quite different after the liposuction, but most importantly, the liposuction lessened her pain and improved her mobility significantly.
Other enticing before-after pictures I've seen have involved the bracelet of fat around the ankle, the "cankles." This is great since many plastic surgeons consider ankles difficult areas and won't do them. They feel there is a lot of critical structure (bone, ligaments, and nerves) around ankles which is prone to damage with traditional liposuction. WAL liposuction, on the other hand, seems to handle them just fine.
Many women with lipedema find that the bracelet of fat is one of the most challenging areas of fat to have. Heavy legs can be covered up with skirts or with pants, but it is difficult to cover up cankles because they are still visible under long skirts and at the bottoms of pants legs.
|
|
Before and After images, Schmeller 2012
|
On a practical basis, having a large cuff of fat at the ankle makes it difficult to find socks or boots that fit. This often means buying short socks and wearing regular shoes instead of boots, even in cold or wet weather. This can result in women walking around with cold or wet feet during the winter, a recipe for hypothermia, frostbite, or skin infections.
If tumescent liposuction can reduce the cankles enough, some women are able to finally wear footwear suitable for bad weather. You can read the story of one woman who was able to fit back into rain boots after having WAL liposuction
here.
|
|
Liposuction result on arms; Schmeller 2012
|
Another lipedema spot that is emotionally challenging to women is the arm. Heavy arms are right by the face, and use of the arms and hands draws people's attention to them more than to legs. People stare at very heavy arms and it can be difficult to regain their focus. As a result, many lipedema women prefer to cover their arms, but it is difficult to find tops with sleeves long enough to cover lipedema fat yet short enough not to overheat in warm weather.
As a result, some lipedema women choose to get liposuction of arm fat, particularly that which is just above the elbow or which hangs down from the upper arm. This can be pretty successful, as seen in the pictures above.
However, it should be noted that not all cases of liposuction are as successful as the pictures shown above. I've seen before and after photos that were rather underwhelming. It's very difficult to guarantee what kind of aesthetic results might
occur.
But remember, the main point of this procedure is NOT aesthetics, it's about improving function, pain levels, mobility, and lessening the risk for further progression of the lipedema.
Research Studies
Pictures can be doctored or cherry-picked for the best cases. What does
the data say about liposuction for lipedema?
Research thus far shows that lymph-sparing tumescent liposuction indeed results in lower pain levels, smaller leg circumferences, less bruising, and improved mobility.
Although there are several studies available, let's focus on discussing the
Schemller study because it is the largest and longest liposuction trial. It involved 112 patients (mostly Stage 2), followed for a mean of about 3.5 years.
Most importantly, women reported a big decrease in pain levels and a reduction in bruising and swelling. Many were able to reduce other treatments,
with 22% able to discontinue all other treatments. Several also reported improvement in mobility after the surgery. (This would probably be even higher if they had had more Stage 3 patients in the study; most were Stage 2, where mobility is not yet that impacted.)
The study found that on average, women lost about 1.5 inches (calves) to 3 inches (thighs) from their leg circumference. The treatment resulted in only very small weight losses, but 74% of women were able to go down between 1 and 3 pants sizes after treatment. That would be very meaningful to many women, and not just for aesthetic reasons.
Complications were minimal. About 1.4% experienced an infection afterwards (minor), similar to levels experienced in other studies of tumescent liposuction. Significant bleeding occurred in 1 patient (0.3%), although the authors note that this is the only patient of theirs who has experienced bleeding in 10 years (1826 patients), for an incidence of 0.05% overall through the years.
The improvements in condition in the women in the study have TREMENDOUS implications for women with lipedema. If further research continues to show improvements like these, then lymph-sparing tumescent liposuction
should be covered by insurance, especially since some women have been able to lessen or even discontinue their complete decongestive therapy after this liposuction.
Liposuction might involve a larger up-front cost, but might actually save money for insurance companies in the long run by lessening the need for complete decongestive therapy, compression garments, and hospitalizations for cellulitis and other complications as the condition progresses.
In fact, the German Society of Phlebology now includes liposuction as part of its guidelines for the treatment of lipedema. Sadly, though, costs for this liposuction are often out of pocket (even in Germany, where the most research has been done). Insurance views liposuction as a strictly cosmetic procedure, and many U.S. insurance companies don't even recognize lipedema as a real condition.
Although a few people have been able to get liposuction for lipedema covered as a medically-necessary procedure, most must pay for it themselves. And since there are only a few surgeons trained in this specialized technique, personal costs often include air fare and hotels in addition to the procedure. This puts it out of reach of most people with lipedema.
Hopefully with time and more research, more insurance companies will see that their bottom lines would benefit by covering this surgery. However, regardless of the bottom line, hopefully they would realize that such a procedure is NOT cosmetic but should be covered because it improves the health and the quality of life of the patient, their customer.
Finding a Qualified Surgeon
It's important to note that many plastic surgeons perform tumescent liposuction, but that doesn't mean they are performing lymph-sparing tumescent liposuction.
Remember, in this version, great care is taken to avoid the lymph system as well as the vascular system so the liposuction does not make things worse. Ordinary tumescent liposuction may not take this kind of care and may use a criss-cross motion that is particularly damaging to the lymph system.
If you are going to consider tumescent liposuction, it's vitally important to get it done by a doctor who specializes in treating lipedema patients, and preferably trained by one of the experts in the field.
A botched operation can result in significant damage to the lymph system and a worsening of the patient's condition. In addition, there are occasional
case reports of other complications as well. You really want to go with a surgeon who has the correct training, plenty of experience, and who works in center capable of handling serious complications if they should occur.
Sadly, only a few doctors are currently trained in this procedure, but more are learning all the time. Until just recently, the main doctors doing this special lipedema liposuction were in Germany so if you wanted this treatment, you had to fly to Germany to get it. Some of the doctors doing it in Germany include:
- Dr. Stefan Rapprich, Rosenberg Klinik in Sonthofen, Germany. He trains other surgeons in this technique
- Dr. Josef Stutz in Bad Steben Germany, one of the leaders in training other doctors in this technique
- Dr. Wilfred Schmeller, Hanse-Klinik in Lübeck, Germany
- Dr. Reggy Schift in Borken Germany; reportedly specializes in people with large volume (lipo-lymphedema), doing a series of surgeries over several weeks
Recently, some British and American doctors have received training on this procedure from the German experts and now offer it. Treatment centers/surgeons for lipedema in the U.S. include:
[Obviously, I do NOT endorse any particular provider or give any feedback on their program, but since there are so few doctors in the world who have trained in this, I felt it was important to pass along some of the possible names. There may be others I am not aware of, and I'm sure there will be more in the next few years as the training program expands. Also, personnel at various clinics may change, so be aware this list will evolve quickly; do your research.]
There may be other doctors who know how to do this procedure, but you need to
consider carefully when choosing a surgeon. The Fat Disorders Research Society has a great
list of questions to consider when choosing a surgeon for lymph-sparing tumescent liposuction.
For example, find out whether your doctor has special training in this procedure for lipedema and who they trained with. You want someone who was trained by some of the leaders in the field, and who knows techniques
specific to lipedema, not just tumescent liposuction in general. How many of these procedures has this person done, where is the surgery performed, how is care handled if there are problems?
Ask about your surgeon's complication rate, post-op management, what services they offer post-op patients, what to do if you experienced complications after returning to your city, etc. Also consider how the doctor approaches you ─ do they ask enough about your medical history, do they care about you as a patient or are they impersonal and cold, do they explain clearly about what you can expect, are they pressuring you into the surgery, etc. Although a good bedside manner does not guarantee a good surgeon, you would hopefully find someone who has both qualities.
Some doctors feel that it is important to do liposuction before the lipedema gets too severe. Some say the most benefit has been seen in women in Stage 2 and early Stage 3 lipedema. Some doctors refuse to do the procedure on women with Stage 4 lipo-lymphedema because they feel it is too complicated with the added lymphedema. On the other hand, there are a few doctors who will work with women who have secondary lymphedema, so never give up looking.
Sadly, weight bias occurs in liposuction treatment too. In the medical literature, some have
promoted liposuction only for lipedemic women "with an acceptable waist measurement." Other women have been
told they must lose some of their "normal" fat first before being able to access liposuction.
Again, as we
discussed recently, it goes back to the biased attitudes of many lipedema providers that if a woman with lipedema is significantly obese, it
must be because she has poor habits, not simply that she has a more severe presentation of the condition. This is a common assumption and shows that even lipedema care providers have not freed themselves from typical weight stereotypes and biases.
There should not be weight limitations for lymph-sparing tumescent liposuction. It is short-sighted and WRONG to keep the potential benefits of liposuction
from the women most in need of it.
Conclusion
Traditional "dry" liposuction and lipectomy are clearly
very bad choices for women with lipedema. They damage the lymph system and often worsen a woman's condition instead of improving it.
Because early attempts with dry liposuction had disastrous results, some in the lipedema community view all liposuction as a discredited treatment. However, recent development of special techniques to help preserve lymph function have re-invigorated liposuction as a potential treatment for lipedema. Although long-term research is still limited in this new field, what we have so far is quite promising.
Although not a cure, lymph-sparing tumescent liposuction/WAL has clearly shown benefit in reducing pain, bruising, limb volume, mobility limitations, and the need for traditional medical treatments in women with Stage 2 lipedema and above.
Basically, liposuction seems to result in a temporary remission of lipedema symptoms. This is huge in a condition that can be relentlessly progressive to the point of eventual immobility. Even if only a few extra years of mobility and pain relief are bought with liposuction, that is a tremendous improvement in a woman's quality of life because lipedema can become so debilitating.
Although longer-term results are limited and we can't
prove that lymph-sparing liposuction is able to slow or even prevent some progression of lipedema, it seems like a logical possibility. Again, this could have tremendous implications for a woman's quality of life and prevention of complications.
At this point, insurance does
not usually cover tumescent liposuction for lipedema, viewing liposuction as simply cosmetic. Hopefully once lipedema's
ICD code is approved and awareness about lipedema improves, more insurance companies will see that a relatively small investment up front may well save them money later on by preventing or lessening costly complications.
Of course, not everyone in the lipedema community is a fan of tumescent liposuction. Some
urge caution about it because it may be just another trendy treatment. Many are reserving judgment until there is more data on its long-term results.
This is a very valid concern. Although the data we have so far is quite promising, there aren't that many studies, and those we do have are small and have a relatively short follow-up. This is a concern about many lipedema treatments, and it is no less valid here.
However, this treatment modality has tremendous potential because it is the only option that really addresses one of the sources of the issue, the dysfunctional fat cells themselves, even if it can't reverse the process. That is why many people in the lipedema community are really excited.
More research is needed, but what data we have so far seems to indicate that lymph-sparing tumescent liposuction is a significant step in the right direction to improve the lives of women with lipedema.
My Opinion
Personally, I was not very impressed with the idea of lymph-sparing tumescent liposuction when I first began researching it, but have become progressively more excited by the possibility as I learned more. I'm sure that viewpoint shows, so beware possible bias.
We do still need more and longer-lasting research before this treatment is widely adopted. I'm also concerned that some plastic surgeons are opportunistic and might see this as the new "cash cow" money-making opportunity. The last thing we need is under-trained surgeons performing liposuction without deep knowledge of lipedema-specific techniques, in inadequate facilities, or with insufficient post-op care. So I do still have reservations about liposuction for lipedema, even as I find it one of the most promising treatment directions for the future.
Another reservation is that all the focus on liposuction might keep researchers from focusing on discovering the underlying causes of lipedema. If we ever hope to truly treat lipedema more effectively, we need to know why it happens. Liposuction only addresses part of the issue, and at best only offers a partial remission.
Lipedema researchers need to do MUCH MORE work on discovering the causes of lipedema, particularly endocrine issues that might be promoting hypertrophy and hyperplasia of the fat cells. All the attention on liposuction must not divert the attention from the basics of learning about this disorder.
Final Thoughts
Although there are still questions to be answered, lymph-sparing liposuction represents one of our best hopes for treating lipedema right now. Most other available treatments, although effective, simply lessen lymph symptoms. Lipedema at least addresses part of the basic problem by getting rid of some of the dysfunctional fat cells themselves.
Liposuction is not a cure, and it doesn't guarantee that the patient won't experience lipedema flares again in the future. However, lymph-sparing liposuction is at least a step in the right direction in reducing the significant morbidity and burden from this disorder.
Now that doctors in the U.K. and the U.S. are beginning to receive training in lymph-sparing liposuction from German doctors, more patients will be helped and more data on it will be collected. If that data is promising, hopefully this training will spread. Women of all countries deserve to have this option without having to travel long distances to get it.
*You can read more about one woman's recent journey through a lymph-sparing tumescent liposuction procedure here. Other women's stories are told here, here, and here. There is a good verbal description of it about 26 minutes into this video, (trigger warning: weight loss talk). There are also informative YouTube videos about liposuction for lipedema from various surgical centers around the U.S., as well as patient testimonials and news stories.
References and Resources
Resources
*Trigger Warning: Many of these sites are not size-friendly. However, because they also contain valuable information about lipedema and its treatment, they are included here.
Lipedema Support Groups
Websites About Those Dealing with Specific Lipedema Treatments
Liposuction Research
British Journal of Dermatology. 2012 Jan;166(1):161-8. doi: 10.1111/j.1365-2133.2011.10566.x. Epub 2011 Nov 17.
Tumescent liposuction in lipodema yields good long-term results. Schmeller, W., Hueppe, M., & Meier-Vollrath, I. PMID:
21824127 Full text
here.
BACKGROUND: ...surgical therapy with tumescent liposuction has only been used for about 10 years and long-term results are unknown...METHODS: A total of 164 patients who had undergone conservative therapy over a period of years, were treated by liposuction under tumescent local anaesthesia with vibrating microcannulas. In a monocentric study, 112 could be re-evaluated with a standardized questionnaire after a mean of 3 years and 8 months (range 1 year and 1 month to 7 years and 4 months) following the initial surgery and a mean of 2 years and 11 months (8 months to 6 years and 10 months) following the last surgery. RESULTS: All patients showed a distinct reduction of subcutaneous fatty tissue (average 9846 mL per person) with improvement of shape and normalization of body proportions. Additionally, they reported either a marked improvement or a complete disappearance of spontaneous pain, sensitivity to pressure, oedema, bruising, restriction of movement and cosmetic impairment, resulting in a tremendous increase in quality of life; all these complaints were reduced significantly (P<0·001). Patients with lipoedema stage II and III showed better improvement compared with patients with stage I. Physical decongestive therapy could be either omitted (22·4% of cases) or continued to a much lower degree. No serious complications (wound infection rate 1·4%, bleeding rate 0·3%) were observed following surgery. CONCLUSIONS: Tumescent liposuction is a highly effective treatment for lipoedema with good morphological and functional long-term results.
J Dtsch Dermatol Ges. 2011 Jan;9(1):33-40. doi: 10.1111/j.1610-0387.2010.07504.x. Epub 2010 Sep 7.
Liposuction is an effective treatment for lipedema-results of a study with 25 patients. [Article in English, German] Rapprich S1, Dingler A, Podda M. PMID:
21166777
...The removal of the increased fat tissue of lipedema has become possible by employing advanced liposuction techniques which utilize vibrating microcannulas under tumescent local anesthesia. The effectiveness of this approach to lipedema is the subject of this study. PATIENTS AND METHODS: 25 patients were examined before liposuction and six months thereafter. The survey included the measurement of the volume of the legs and several parameters of typical pain and discomfort. The parameters were measured using visual analogue scales (VAS, scale 0-10). RESULTS: The volume of the leg was reduced by 6.99 %. Pain, as the predominant symptom in lipedema, was significantly reduced from 7.2 ± 2.2 to 2.1 ± 2.1 (p < 0.001). Quality of life as a measure of the psychological strain caused by lipedema improved from 8.7 ± 1.7 to 3.6 ± 2.5 (p < 0.001). Other parameters also showed a significant improvement and the over-all severity score improved in all patients. CONCLUSION: Liposuction reduces the symptoms of lipedema significantly.
J Cutan Med Surg. 2006 Jan-Feb;10(1):7-10.
Tumescent liposuction: a new and successful therapy for lipedema. Schmeller W1, Meier-Vollrath I. PMID:
17241565
...Twenty-eight patients, who had undergone conservative therapy over a period of years, were treated by liposuction under tumescent local anesthesia with vibrating microcannulas. Twenty-one could be reevaluated after an average of 12.2 (1-26) months. RESULTS: All showed great improvement, with normalization of body proportions. Additionally, spontaneous pain, sensitivity to pressure, and bruising either disappeared completely or improved markedly. Other than minor swelling for a few days, no complications could be observed following surgery. All patients reported a tremendous increase in their quality of life. Physical therapy had to be continued to a much lower degree. CONCLUSION: Tumescent liposuction has proved to be a safe and effective treatment for lipedema.
Clin Cosmet Investig Dermatol. 2014 Jan 23;7:35-42. doi: 10.2147/CCID.S56655. eCollection 2014.
Treatment of elderly patients with advanced lipedema: a combination of laser-assisted liposuction, medial thigh lift, and lower partial abdominoplasty. Wollina U1, Heinig B2, Nowak A3. PMID:
24489474 Full text available
here.
...In advanced stages, reduction of adipose tissue is the only available effective treatment [for lipedema]. In elderly patients with advanced lipedema, correction of increased skin laxity has to be considered for an optimal outcome. METHODS: We report on a tailored combined approach to improve advanced lipedema in elderly females with multiple comorbidities. Microcannular laser-assisted liposuction of the upper legs and knees is performed under tumescent anesthesia. Medial thigh lift and partial lower abdominoplasty with minimal undermining are used to correct skin laxity and prevent intertrigo. Postsurgical care with nonelastic flat knitted compression garments and manual lymph drainage are used. RESULTS: We report on three women aged 55-77 years with advanced lipedema of the legs and multiple comorbidities. Using this step-by-step approach, a short operation time and early mobilization were possible. Minor adverse effects were temporary methemoglobinemia after tumescent anesthesia and postsurgical pain. No severe adverse effects were seen. Patient satisfaction was high. CONCLUSION: A tailored approach may be useful in advanced lipedema and is applicable even in elderly patients with multiple comorbidities.
Wien Med Wochenschr. 2015 May;165(9-10):189-194. Epub 2015 Jan 21.
Acute pulmonary edema following liposuction due to heart failure and atypical pneumonia. Wollina U1, Graf A, Hanisch V. PMID:
25875251
Microcannular liposuction in tumescent anesthesia is the most effective treatment for painful lipedema. Tumescent anesthesia is an established and safe procedure in local analgesia when performed according to guidelines. Major adverse effects are rare. In patients with advanced lipedema, however, the commonly presented comorbidities bear additional risks.We report on post-surgical acute pulmonary edema after tumescent liposuction according to guidelines in a 52-year-old female patient with lipedema of the legs. We discuss in detail possible scenarios that might be involved in such emergency. In the present case the most likely was a retarded community acquired atypical pneumonia with aggravation of pre-existent comorbidities.A combined treatment with intravenous b-lactam antibiosis, positive pressure ventilation, and continuous venovenous hemodialysis and filtration resulted in complete remission in a couple of days. In conclusion, tumescent liposuction of advanced lipedema patients should only be performed in well-trained centers with sufficient infrastructure.
Ann Plast Surg. 2012 Mar;68(3):303-7. doi: 10.1097/SAP.0b013e318215791e.
Long-term Outcome After Surgical Treatment of Lipedema. Peled AW1, Slavin SA, Brorson H. PMID:
21629090
...We report a case of a patient with lipedema who was treated with suction-assisted lipectomy and use of compression garments, with successful treatment of the lipodystrophy and maintenance of improved aesthetic results at 4-year postoperative follow-up.